Pain hypersensitivity and many other diseases could be associated with a protein that acts as an ion pump in neurons.
The research team led by Yves De Koninck, at Université Laval’s Faculté de médecine and the CERVO Brain Research Centre had already targeted a protein called KCC2 as a key player in the mechanism leading to pain hypersensitivity. A new study published last week in Nature Communications confirms confirms this lead and reinforces the idea that this protein could be a target of choice for the creation of a new class of analgesics to treat this problem that medicine is often powerless to address.
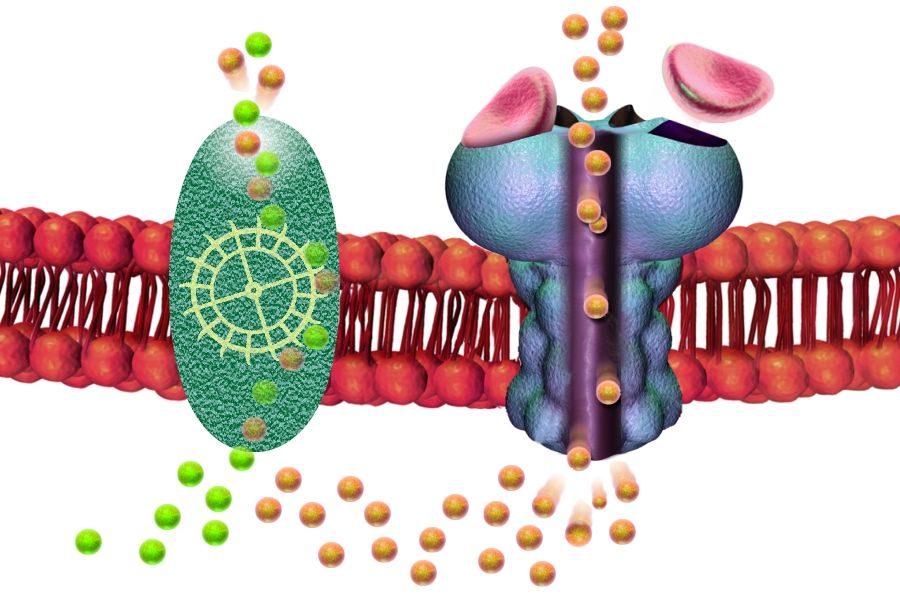
The KCC2 transporter is a protein that controls the balance of ions between the inside and outside of neurons. When this pump does not work properly, chloride ions accumulate in the neurons, making them more easily excitable. “KCC2 is involved in the gate system that determines whether a painful signal from the sensory nerves is relayed to the brain or not by the neurons in the spinal cord,” says Professor De Koninck. Its role is to inhibit the transmission of the pain signal. Without this protein, the gate no longer functions and pain signals are constantly relayed to the brain.”
His team had already shown that a lack of KCC2 explained why the effectiveness of morphine against neuropathic pain decreased over time and why its prolonged use could even increase pain sensitivity. In their latest paper, the researchers show that KCC2 also plays a role in another paradoxical phenomenon associated with another class of drugs, benzodiazepines.
These drugs – including Valium and Ativan – are among the most widely prescribed drugs in the world for anxiety, insomnia, psychomotor agitation, spasms and epilepsy. “The administration of a massive dose of benzodiazepines is the recommended treatment when a person has a major epileptic seizure,” says Professor De Koninck. Paradoxically, these drugs can cause serious problems if used in newborns suffering from this disease. They may even increase the risk of epileptic seizures.”
In an attempt to elucidate this paradox, researchers examined what happens when a benzodiazepine analog was administered to mice after sensory nerve damage. At high doses, this molecule fails to induce analgesia because the expulsion of chloride ions out of the cell is not done properly by KCC2,” explains the researcher. By injecting mice with a product that increases the activity of this transporter, we restore its analgesic effect. Disruption of this pump could also be responsible for chronic stress, anxiety, epilepsy, autism, schizophrenia, spasms associated with spinal cord injury and some neurodegenerative diseases” says Yves De Koninck
The search for molecules that can increase the activity of KCC2 continues. “We have a new family of molecules that we have patented against pain hypersensitivity and we hope to find funding to test them. Our work suggests that the proper functioning of this transporter in maintaining homeostasis of chloride ions goes beyond the issue of chronic pain. It may also be involved in chronic stress, anxiety, epilepsy, autism, schizophrenia, spasms associated with spinal cord injury and certain neurodegenerative diseases.”
The other signatories of the study are, at Laval University, Louis-Étienne Lorenzo, Antoine Godin, Francesco Ferrini, Karine Bachand, Isabel Plasencia-Fernandez, Simon Labrecque, Alexandre Girard, Dominic Boudreau, Martin Gagnon and Nicolas Doyon, and at McGill University, Irenej Kianicka and Alfredo Ribeiro-da-Silva.
The french version of this article was published in Le fil de l’Université Laval
Read the original research article.
Louis-Etienne Lorenzo, Antoine G. Godin, Francesco Ferrini, Karine Bachand, Isabel Plasencia-Fernandez, Simon Labrecque, Alexandre A. Girard, Dominic Boudreau, Irenej Kianicka, Martin Gagnon, Nicolas Doyon, Alfredo Ribeiro-da-Silva & Yves De Koninck Enhancing neuronal chloride extrusion rescues α2/α3 GABAA-mediated analgesia in neuropathic pain. Nat Commun 11, 869 (2020). https://doi.org/10.1038/s41467-019-14154-6